Flat flow limitation graph?
Flat flow limitation graph?
Do any/some/most people actually have flat flow limitation graphs? Is that even possible? Or is it the case that EVERYONE has spikes throughout the night?
_________________
| Mask: Eson™ Nasal CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
Re: Flat flow limitation graph?
When I was using the S9 I routinely saw these boring flow limitation graphs or even some with even less little blips.
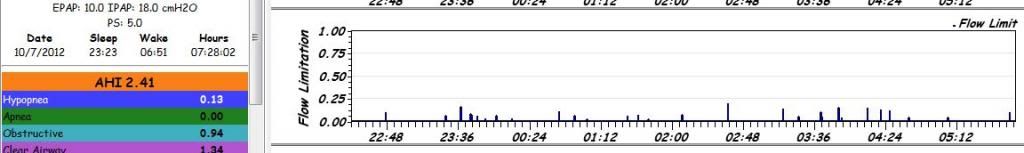
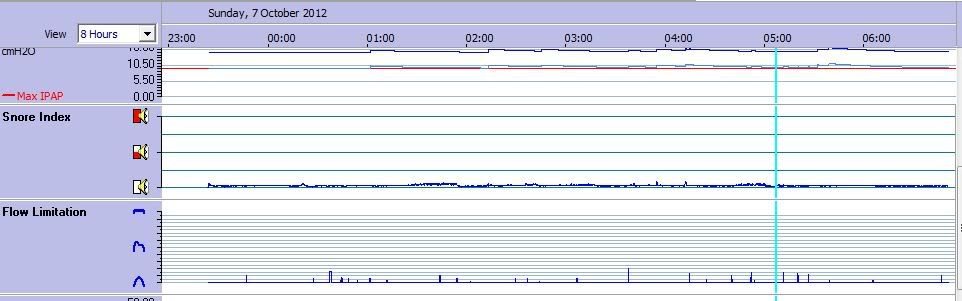
this one has pretty flat.
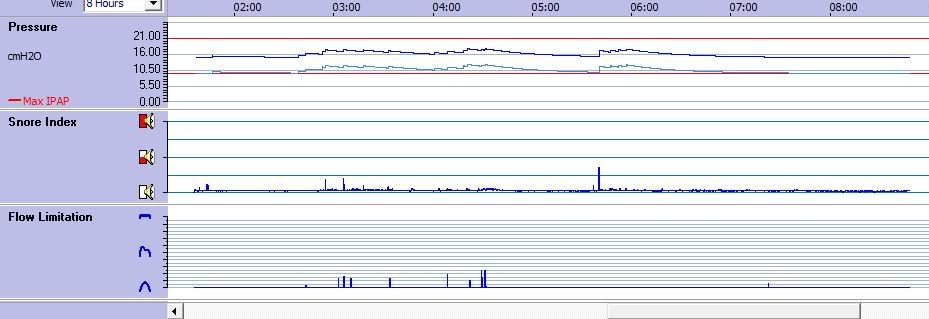


this one has pretty flat.

_________________
| Machine: AirCurve™ 10 VAuto BiLevel Machine with HumidAir™ Heated Humidifier |
| Additional Comments: Mask Bleep Eclipse https://bleepsleep.com/the-eclipse/ |
I may have to RISE but I refuse to SHINE.
Re: Flat flow limitation graph?
Thanks Pugsy! I'm trying to increase pressure a bit to see if I can iron out some flow limitations, and wondered what the "goal" should be in terms of the graph.
_________________
| Mask: Eson™ Nasal CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
Re: Flat flow limitation graph?
I don't know if what I get is necessarily the "goal" but I have been fortunate that Flow Limitations haven't been something I have ever had very many of.
Remember for years I used a Respironics machine and the way that they report Flow Limitations is totally different from the S9's graphs. I didn't know how really boring my FLs were until I saw mine and saw some other people's graphs which showed a lot of activity.
Remember for years I used a Respironics machine and the way that they report Flow Limitations is totally different from the S9's graphs. I didn't know how really boring my FLs were until I saw mine and saw some other people's graphs which showed a lot of activity.
_________________
| Machine: AirCurve™ 10 VAuto BiLevel Machine with HumidAir™ Heated Humidifier |
| Additional Comments: Mask Bleep Eclipse https://bleepsleep.com/the-eclipse/ |
I may have to RISE but I refuse to SHINE.
-
Wulfman...
Re: Flat flow limitation graph?
Your profile shows you're using an Elite......a single pressure machine. Since Flow Limitations are one of the things that Auto CPAP machines use to trigger pressure increases, it's possible that that feature is not functional in your machine reports.Iowamv wrote:Do any/some/most people actually have flat flow limitation graphs? Is that even possible? Or is it the case that EVERYONE has spikes throughout the night?
At least that's the way it is for Respironics machines running in single pressure mode.
Den
.
Re: Flat flow limitation graph?
Hey Den,
The ResMed S9 flags Flow Limitations in the form of the graph that I showed above from my S9 in the fixed pressure modes as well as auto adjusting modes.
It's not like the Respironics machines ignoring FLs in cpap mode. The S9 ELite will record FLs even if they can't do anything about them. FL graphs are also flagged with the S9 VPAP in S mode (fixed bilevel).
The ResMed S9 flags Flow Limitations in the form of the graph that I showed above from my S9 in the fixed pressure modes as well as auto adjusting modes.
It's not like the Respironics machines ignoring FLs in cpap mode. The S9 ELite will record FLs even if they can't do anything about them. FL graphs are also flagged with the S9 VPAP in S mode (fixed bilevel).
_________________
| Machine: AirCurve™ 10 VAuto BiLevel Machine with HumidAir™ Heated Humidifier |
| Additional Comments: Mask Bleep Eclipse https://bleepsleep.com/the-eclipse/ |
I may have to RISE but I refuse to SHINE.
-
Wulfman...
Re: Flat flow limitation graph?
OK. Thanks for the info.Pugsy wrote:Hey Den,
The ResMed S9 flags Flow Limitations in the form of the graph that I showed above from my S9 in the fixed pressure modes as well as auto adjusting modes.
It's not like the Respironics machines ignoring FLs in cpap mode. The S9 ELite will record FLs even if they can't do anything about them. FL graphs are also flagged with the S9 VPAP in S mode (fixed bilevel).
Could it be that he just doesn't have many flow limitations........or a consistent number of them? (causing the "flat" graph)
Den
.
Re: Flat flow limitation graph?
No...those graphs are mine not OP here. I haven't seen his FL graphs from his S9 (at least that I remember).Wulfman... wrote:Could it be that he just doesn't have many flow limitations........or a consistent number of them? (causing the "flat" graph)
I get the impression that his FL graphs are quite active and he was wondering if anyone ever got flat or close to flat FL graphs...so I showed him mine because they are about as boring as they come.
I assume that his FL graphs are probably pretty ugly ( to his thinking ) and he is thinking (correctly) that a little more pressure might help reduce the FLs.
I think he is wanting to try to get his FL graphs to maybe look a little more like mine.
_________________
| Machine: AirCurve™ 10 VAuto BiLevel Machine with HumidAir™ Heated Humidifier |
| Additional Comments: Mask Bleep Eclipse https://bleepsleep.com/the-eclipse/ |
I may have to RISE but I refuse to SHINE.
Re: Flat flow limitation graph?
Hi Den,
I've definitely got spikes, sometimes in clusters. Just wondered how many of them most people consider normal.
Thanks.
I've definitely got spikes, sometimes in clusters. Just wondered how many of them most people consider normal.
Thanks.
_________________
| Mask: Eson™ Nasal CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
-
Wulfman...
Re: Flat flow limitation graph?
From my understanding, the usual "remedy" for flow limitations is a little more pressure. Your profile doesn't say what pressure or EPR setting you're using, so it's kind of hard to say what to recommend......other than to try reducing your EPR setting (if you're using it) and/or bump up your pressure a bit to see if it makes a difference.Iowamv wrote:Hi Den,
I've definitely got spikes, sometimes in clusters. Just wondered how many of them most people consider normal.
Thanks.
Den
.
Re: Flat flow limitation graph?
Can you show us a picture of a typical flow limitation graph that you are seeing?
Maybe it really isn't all that bad and not worth worrying about????
Maybe it really isn't all that bad and not worth worrying about????
_________________
| Machine: AirCurve™ 10 VAuto BiLevel Machine with HumidAir™ Heated Humidifier |
| Additional Comments: Mask Bleep Eclipse https://bleepsleep.com/the-eclipse/ |
I may have to RISE but I refuse to SHINE.
-
Wulfman...
Re: Flat flow limitation graph?
Another possibility could be that it's "positional". Something in your sleeping position that's causing the clusters/spikes.
Den
.
Den
.
Re: Flat flow limitation graph?
During my first year in 2011 I used S9 Elite, and after a year S9 Autoset mostly on APAP. My Flow Limitation (FL) graph on the S9 Elite with pressures varying from 7 cm to 17 cm kept constant around the mid level. On the S9 Autoset in APAP mode the graph has been half as high.
Here is a recent example, from Aug 2013, on the S9 Autoset at APAP:

This is the pressure graph on it:

The following are my graphs on the S9 Elite from 2011, and they were lousy:

Besides, there is not much that you can do to reduce the FL much. See this report:
About UARs (Upper Airway Resistance syndrome, is included in Resmed’s machines Flow Limitation graphs)
As of 07.01.2011
Treatment
The optimal treatment for patients with UARS is not currently known. Continuous positive airway pressure (CPAP) has been quite useful in the treatment of sleep-disordered breathing and there are some notable positive results in CPAP treatment of UARS. In a study of 15 heavy snorers with clinical evidence of UARS, treatment with nasal CPAP was associated with decreases in observed nocturnal arousals on polysomnography and decreases in mean sleep latency times on multiple sleep latency testing (MSLT) after several nights of treatment.3,36 A follow-up study of 15 subjects (in the original description of UARS) with daytime sleepiness and fatigue and who had undergone a therapeutic trial of positive pressure therapy reported similar findings.3 After treatment with approximately a month of nasal CPAP, significant improvements were seen in mean sleep latency times on MSLT (5.3 minutes vs 13.5 minutes), Pes nadir pressure (–33.1 cm H2O vs –5.3 cm H2O), amount of slow-wave sleep (1.2% vs 9.7%), and EEG arousals (31.3 vs 7.9 events/hour of sleep). Along with an improvement in sleep latency times on MSLT, there were subjective reports of improved daytime symptoms. Lastly, in a study of 130 postmenopausal women with chronic insomnia and evidence of UARS (n=62) or normal breathing (n=68), treatment with either nasal turbinectomy or nasal CPAP was associated with improvements in subjective reports of sleep quality as measured with a visual analog scale as well as mean sleep latency times on polysomnography.19 Despite the growing body of evidence supporting the use of positive pressure therapy for UARS patients, it remains difficult to obtain therapy. In a follow-up study of more than 90 patients conducted 4 to 5 years after the initial diagnosis of UARS was made, none of the subjects were receiving CPAP treatment; the main rationale given was that their insurance provider declined to provide the necessary equipment.1 Formal follow-up clinical evaluations of these patients noted significant worsening in their sleep-related complaints, with increased reports of fatigue, insomnia, and depressive mood. More disturbingly, prescriptions for hypnotics, stimulants, and antidepressants increased more than fivefold.
Other interventions, such as surgery or oral appliances, have also been used with some success in the treatment of patients with UARS. Procedures such as uvulopalatopharyngoplasty, laser-assisted uvuloplasty (LAUP), septoplasty with turbinate reduction, genioglossus advancement, and radiofrequency ablation of the palate have all been described in the literature.37-40 A study of LAUP in nine patients with UARS who underwent uvulopalatopharyngoplasty (n=2), multilevel pharyngeal surgery (n=1), or LAUP (n=6) reported improvements in subjective daytime sleepiness as measured with Epworth Sleepiness Scale scores.37 In the two patients for whom postoperative polysomnographic data was available, significant improvements in Pes nadir pressures were seen. But patients had several interventions and it is difficult to assess which one was successful. A study of 14 patients with UARS who underwent radiofrequency ablation of the palate also reported improvement in subjective sleepiness, with concurrent improvements in Pes nadir levels and reports of snoring.40 However, prior reviews of the available literature have noted that many of the studies evaluated small numbers of patients, consisted of uncontrolled case reports or series without clear characterization of the subjects enrolled, and had no consistent end points for an adequate evaluation of efficacy.39 Further investigation is required to determine the specific role for surgical intervention in these patients. Other authors have also reported successful treatment of UARS with use of oral appliances, although these studies suffer from the same limitations as the surgical literature.41 In children, orthodontic approaches, such as maxillary distraction or use of expanders, have also shown promising results.42
Abbreviations:
CAP = cyclical alternating pattern; CPAP = continuous positive airway pressure; LAUP = laser-assisted uvuloplasty; MSLT = multiple sleep latency testing; NREM = nonrapid eye movement; OHS = obstructive hypopnea syndrome; OSAS = obstructive sleep apnea syndrome; Pes = esophageal pressure; REM = rapid eye movement; RERA = respiratory effort-related arousal; UARS = upper airway resistance syndrome
Source:
http://www.chestnet.org/accp/pccsu/uppe ... e?page=0,3
This link does not work anymore. I think that they stopped the free access.
But you can see it here:
http://www.apneaboard.com/forums/Thread ... e-Syndrome

Here is a recent example, from Aug 2013, on the S9 Autoset at APAP:

This is the pressure graph on it:

The following are my graphs on the S9 Elite from 2011, and they were lousy:

Besides, there is not much that you can do to reduce the FL much. See this report:
About UARs (Upper Airway Resistance syndrome, is included in Resmed’s machines Flow Limitation graphs)
As of 07.01.2011
Treatment
The optimal treatment for patients with UARS is not currently known. Continuous positive airway pressure (CPAP) has been quite useful in the treatment of sleep-disordered breathing and there are some notable positive results in CPAP treatment of UARS. In a study of 15 heavy snorers with clinical evidence of UARS, treatment with nasal CPAP was associated with decreases in observed nocturnal arousals on polysomnography and decreases in mean sleep latency times on multiple sleep latency testing (MSLT) after several nights of treatment.3,36 A follow-up study of 15 subjects (in the original description of UARS) with daytime sleepiness and fatigue and who had undergone a therapeutic trial of positive pressure therapy reported similar findings.3 After treatment with approximately a month of nasal CPAP, significant improvements were seen in mean sleep latency times on MSLT (5.3 minutes vs 13.5 minutes), Pes nadir pressure (–33.1 cm H2O vs –5.3 cm H2O), amount of slow-wave sleep (1.2% vs 9.7%), and EEG arousals (31.3 vs 7.9 events/hour of sleep). Along with an improvement in sleep latency times on MSLT, there were subjective reports of improved daytime symptoms. Lastly, in a study of 130 postmenopausal women with chronic insomnia and evidence of UARS (n=62) or normal breathing (n=68), treatment with either nasal turbinectomy or nasal CPAP was associated with improvements in subjective reports of sleep quality as measured with a visual analog scale as well as mean sleep latency times on polysomnography.19 Despite the growing body of evidence supporting the use of positive pressure therapy for UARS patients, it remains difficult to obtain therapy. In a follow-up study of more than 90 patients conducted 4 to 5 years after the initial diagnosis of UARS was made, none of the subjects were receiving CPAP treatment; the main rationale given was that their insurance provider declined to provide the necessary equipment.1 Formal follow-up clinical evaluations of these patients noted significant worsening in their sleep-related complaints, with increased reports of fatigue, insomnia, and depressive mood. More disturbingly, prescriptions for hypnotics, stimulants, and antidepressants increased more than fivefold.
Other interventions, such as surgery or oral appliances, have also been used with some success in the treatment of patients with UARS. Procedures such as uvulopalatopharyngoplasty, laser-assisted uvuloplasty (LAUP), septoplasty with turbinate reduction, genioglossus advancement, and radiofrequency ablation of the palate have all been described in the literature.37-40 A study of LAUP in nine patients with UARS who underwent uvulopalatopharyngoplasty (n=2), multilevel pharyngeal surgery (n=1), or LAUP (n=6) reported improvements in subjective daytime sleepiness as measured with Epworth Sleepiness Scale scores.37 In the two patients for whom postoperative polysomnographic data was available, significant improvements in Pes nadir pressures were seen. But patients had several interventions and it is difficult to assess which one was successful. A study of 14 patients with UARS who underwent radiofrequency ablation of the palate also reported improvement in subjective sleepiness, with concurrent improvements in Pes nadir levels and reports of snoring.40 However, prior reviews of the available literature have noted that many of the studies evaluated small numbers of patients, consisted of uncontrolled case reports or series without clear characterization of the subjects enrolled, and had no consistent end points for an adequate evaluation of efficacy.39 Further investigation is required to determine the specific role for surgical intervention in these patients. Other authors have also reported successful treatment of UARS with use of oral appliances, although these studies suffer from the same limitations as the surgical literature.41 In children, orthodontic approaches, such as maxillary distraction or use of expanders, have also shown promising results.42
Abbreviations:
CAP = cyclical alternating pattern; CPAP = continuous positive airway pressure; LAUP = laser-assisted uvuloplasty; MSLT = multiple sleep latency testing; NREM = nonrapid eye movement; OHS = obstructive hypopnea syndrome; OSAS = obstructive sleep apnea syndrome; Pes = esophageal pressure; REM = rapid eye movement; RERA = respiratory effort-related arousal; UARS = upper airway resistance syndrome
Source:
http://www.chestnet.org/accp/pccsu/uppe ... e?page=0,3
This link does not work anymore. I think that they stopped the free access.
But you can see it here:
http://www.apneaboard.com/forums/Thread ... e-Syndrome
_________________
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: S9 Autoset machine; Ruby chinstrap under the mask straps; ResScan 5.6 |
see my recent set-up and Statistics:
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png