ResMed / ResScan interpretation challenge
ResMed / ResScan interpretation challenge
Question to those of you savvy with interpreting your data on your PC: have you ever tried the tests below as a learning exercise?
Rather than interpreting what the various created curves mean, I thought I'd perform a sanity check and purposely create a few "disturbances". Using either the FX Nasal Pillows or the Quattro FX FF mask.
My therapy problem seems to be mainly cumulative nasal congestion after a couple of hours of sleep, which leads to upper airway restriction, then to flow limitation, which raises the Autoset pressure, creates leakage ... and so on in a vicious circle... on certain unpredictable nights.
So let's see what correlation exists between inputs and outputs at known recording times:
1. in addition to the intended nasal breathing, I took three deep oral breaths
2. I created mask leakage
3. I tried to create flow limitation by pressing on the nasal cavities or on the mask
Well, the oral hyperventilation clearly shows up in the FLOW curves. But I see very little effect of the other "tweaks" when I look in the FLOW, FLOW LIMITATION, or LEAK output. Even after I realized that the clock in the flow generator is 10 min behind the wall clock.
Rather than interpreting what the various created curves mean, I thought I'd perform a sanity check and purposely create a few "disturbances". Using either the FX Nasal Pillows or the Quattro FX FF mask.
My therapy problem seems to be mainly cumulative nasal congestion after a couple of hours of sleep, which leads to upper airway restriction, then to flow limitation, which raises the Autoset pressure, creates leakage ... and so on in a vicious circle... on certain unpredictable nights.
So let's see what correlation exists between inputs and outputs at known recording times:
1. in addition to the intended nasal breathing, I took three deep oral breaths
2. I created mask leakage
3. I tried to create flow limitation by pressing on the nasal cavities or on the mask
Well, the oral hyperventilation clearly shows up in the FLOW curves. But I see very little effect of the other "tweaks" when I look in the FLOW, FLOW LIMITATION, or LEAK output. Even after I realized that the clock in the flow generator is 10 min behind the wall clock.
Moderate-severe OSA, ResMed S9 AutoSet EPR + H5i Humidifier, ResMed Masks: trying Swift FX Nasal Pillow, Mirage Nasal, Mirage Quatro or Quattro FX Full Face
ResMed SD card & USB adaptor, ResScan 3.10
ResMed SD card & USB adaptor, ResScan 3.10
- billbolton
- Posts: 2264
- Joined: Wed Jun 07, 2006 7:46 pm
- Location: Sydney, Australia
Re: ResMed / ResScan interpretation challenge
All xPAP machines are designed to work while you are in a state of autonomous sleep breathing. Anything you do with them will you are awake, including contrived "tests", is outside of the operational parameters, so any results/data are quite meaningless in terms of what would happen during autonomous sleep breathing.AMUW wrote:have you ever tried the tests below as a learning exercise?
Cheers,
Bill
Re: ResMed / ResScan interpretation challenge
Hi Bill, I do have some understanding of the nervous system, in particular I can distinguish between:billbolton wrote:All xPAP machines are designed to work while you are in a state of autonomous sleep breathing
- Central Nervous System: which includes voluntary control of movement
- Peripheral Nervous System, which includes the autonomic nervous system http://en.wikipedia.org/wiki/Autonomic_nervous_system , which in turn includes the balance between sympathetic and parasympathetic parts during sleep respiration; which as you say one doesn't consciously control.
And you're putting your finger on my main problem: my system is fighting CPAP, and apparently only CPAP, with nasal congestion; and I don't seem to be able to do anything about it consciously... to bring CPAP within the compliance range.
Whether it involves anatomic, mechanical, conscious or unconscious neural, or metabolic phenomena, I must test parameters to see which outcomes are most sensitive to which changes. And I can try to recognize whether a cluster of apneas "hitting me" after a few hours of sleep:
- could be due to mask leakage or oral breathing
- whether the mask leakage or the nasal congestion (flow limitation) come first
- whether my ResMed S9 Autoset algorithm raising the pressure upon sensing the above is desirable or not; whether it is possible to get caught in an unstable loop (in this context I've seen the term "vicious circle" being used)
- whether my apnea clusters (like 10-20 coming on within 30 min, and consequent sleep fragmentation) are due to the S9 pressure increase or to the flow limitation, or whether the pre-CPAP OSA is made worse by the treatment
Thanks for listening.
Last edited by AMUW on Sun Mar 20, 2011 6:47 pm, edited 1 time in total.
Moderate-severe OSA, ResMed S9 AutoSet EPR + H5i Humidifier, ResMed Masks: trying Swift FX Nasal Pillow, Mirage Nasal, Mirage Quatro or Quattro FX Full Face
ResMed SD card & USB adaptor, ResScan 3.10
ResMed SD card & USB adaptor, ResScan 3.10
Re: ResMed / ResScan interpretation challenge
Wikipedia isn't a real resource in anyone's world......it may give you some ideas of parameters and outer limits within to search, but is otherwise flawed as a resource.
I agree with Bill Bolton....your results will be as contrived as your simulations.
You must have too much time on your hands............
Consider volunteering with a worthy cause
I agree with Bill Bolton....your results will be as contrived as your simulations.
You must have too much time on your hands............
Consider volunteering with a worthy cause
_________________
| Mask: AirFit™ P10 Nasal Pillow CPAP Mask with Headgear |
| Additional Comments: ResScan software 3.13, Pressure 21/15 |
“Life is 10% what happens to you, and 90% what you make of it.” Charles Swindoll
Re: ResMed / ResScan interpretation challenge
AMUW, You may be looking in the wrong place and over-complicating things.
Most people have to play around with the humidifer settings on the S9 to avoid this. It's a common issue that is well-documented here.AMUW wrote:...
My therapy problem seems to be mainly cumulative nasal congestion after a couple of hours of sleep, which leads to upper airway restriction, then to flow limitation, which raises the Autoset pressure, creates leakage ... and so on in a vicious circle... on certain unpredictable nights.
....
Ray
Diagnosed in 1997
Diagnosed in 1997
-
HoseCrusher
- Posts: 2744
- Joined: Tue Oct 12, 2010 6:42 pm
Re: ResMed / ResScan interpretation challenge
AMUW, Here is how you can set up a test like you are wanting to conduct.
While there may be some controversy over what the results will indicate, I think you can get a general idea of what you are looking for.
If you look at a flow rate report you can pick 10 - 20 minutes of an "average" rate. This will give you a respiration rate. Practice breathing at this rate until you have it down reasonable well.
Next arrange for a quite time to run your test. I suggest that you run at at about 2 pm in the afternoon. This is a perfect nap time.
Lie down in bed and establish your breathing rate that you practiced earlier. Now throw in the various efforts at creating artificial events. Relax further and if you happen to actually fall asleep and take a nap, great. This will give you both "artificial" and real sleep to compare. If you happen to have a pulse oximeter, wear it and strive to achieve a similar pulse rate to what you have when your are sleeping.
You will end up with 1 data point. Repeat this a few times and you may actually be able to find a trend.
While there may be some controversy over what the results will indicate, I think you can get a general idea of what you are looking for.
If you look at a flow rate report you can pick 10 - 20 minutes of an "average" rate. This will give you a respiration rate. Practice breathing at this rate until you have it down reasonable well.
Next arrange for a quite time to run your test. I suggest that you run at at about 2 pm in the afternoon. This is a perfect nap time.
Lie down in bed and establish your breathing rate that you practiced earlier. Now throw in the various efforts at creating artificial events. Relax further and if you happen to actually fall asleep and take a nap, great. This will give you both "artificial" and real sleep to compare. If you happen to have a pulse oximeter, wear it and strive to achieve a similar pulse rate to what you have when your are sleeping.
You will end up with 1 data point. Repeat this a few times and you may actually be able to find a trend.
_________________
| Mask: Brevida™ Nasal Pillow CPAP Mask with Headgear |
| Additional Comments: Machine is an AirSense 10 AutoSet For Her with Heated Humidifier. |
SpO2 96+% and holding...
Re: ResMed / ResScan interpretation challenge
Hi Bill, how can CPAPs detect that you're in autonomous sleep breathing (or test sleep architecture) if it lacks the sensors to do that?billbolton wrote:All xPAP machines are designed to work while you are in a state of autonomous sleep breathing. Anything you do with them will you are awake, including contrived "tests", is outside of the operational parameters, so any results/data are quite meaningless in terms of what would happen during autonomous sleep breathing.AMUW wrote:have you ever tried the tests below as a learning exercise?
Cheers,
Bill
_________________
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: S9 Autoset machine; Ruby chinstrap under the mask straps; ResScan 5.6 |
see my recent set-up and Statistics:
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png
Re: ResMed / ResScan interpretation challenge
They don't. That's why all data collected by the machine while you are awake is of minimal, if any, value. You know, like the central apneas my S9 reports me having while I'm lying in the bed after waking up in the morning, just enjoying the comfort of the pillow and quilt and too lazy to yank the hose off and reach over and turn the machine off.avi123 wrote:Hi Bill, how can CPAPs detect that you're in autonomous sleep breathing (or test sleep architecture) if it lacks the sensors to do that?
_________________
| Mask: AirFit™ P10 Nasal Pillow CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: Hose management - rubber band tied to casement window crank handle! Hey, it works! S/W is 3.13, not 3.7 |
Re: ResMed / ResScan interpretation challenge
Some of the newest FIsher and Paykel machines have a SensAwake feature that is supposed to detect when the user awakens (from changes in breathing patterns) and reduce the output pressure.
Some members have reported that they very much like this feature.
Some members have reported that they very much like this feature.
_________________
| Machine: DreamStation BiPAP® Auto Machine |
| Mask: DreamWear Nasal CPAP Mask with Headgear |
jeff
- billbolton
- Posts: 2264
- Joined: Wed Jun 07, 2006 7:46 pm
- Location: Sydney, Australia
Re: ResMed / ResScan interpretation challenge
You probably need to be videoing yourself while asleep, to see what is physically happeningAMUW wrote:I can try to recognize whether a cluster of apneas "hitting me" after a few hours of sleep:
- could be due to mask leakage or oral breathing
- whether the mask leakage or the nasal congestion (flow limitation) come first
Without some additional data points beyond what an S9 (or pretty much any xPAP) can reasonably determine from flow sensing while you are asleep, you are simply going to be guessing.
Cheers,
Bill
Re: ResMed / ResScan interpretation challenge
Thanks for the comments above. For me this isn't just idle musing: I hope that the discussion leads to some insight.
Between clearly defined sleep and being awake and conscious I see a transition phase. In my case home CPAP records the majority of events at sleep onset nowadays. As shown in the image
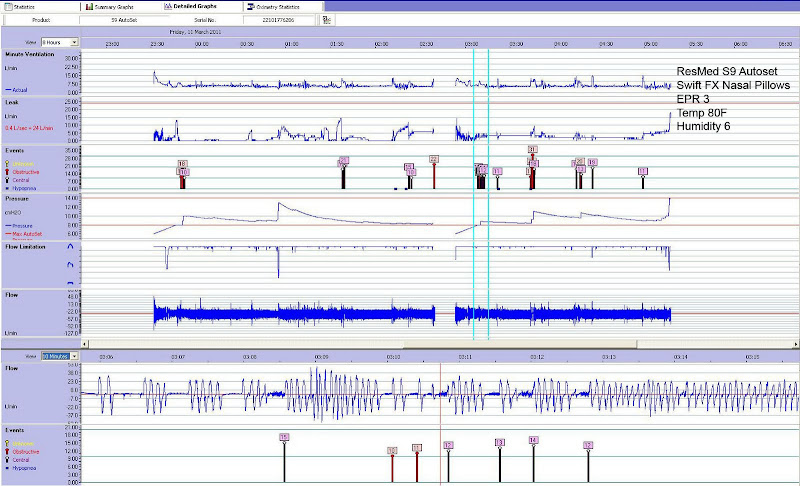
(Mar.22: I need to improve on my first BB attempt to include JPG curves stored elsewhere; Picasa allows me only 800x500 px max resolution).
Should I ignore such a time period as not contributing to OSA, to desaturation, or to sleep fragmentation? Still I see a correlation between subjective accumulated sleep and the duration of sleep onset apnea cluster.
My PSG studies found that I was spending a lot of night time not in N-stages or REM-stage, but in the W(wake)-stage. And it didn't count events during this unconscious, but non-sleep stage. My home CPAP can't differentiate sleep stages, so it counts all events it can identify during total recording time.avi123 wrote:Hi Bill, how can CPAPs detect that you're in autonomous sleep breathing (or test sleep architecture) if it lacks the sensors to do that?
idamtnboy, I sometime get what ResMed S9 classifies as apnea clusters (OAs or CAs intermixed) even before I fully fall asleep. Here is a extract that you could compare to: does your final phase go in & out of consciousness, like my Sleep Onset?idamtnboy wrote:data collected by the machine while you are awake is of minimal, if any, value...like the central apneas my S9 reports me having while I'm lying in the bed after waking up in the morning, just enjoying the comfort of the pillow and quilt and too lazy to yank the hose off and reach over and turn the machine off.
Between clearly defined sleep and being awake and conscious I see a transition phase. In my case home CPAP records the majority of events at sleep onset nowadays. As shown in the image

(Mar.22: I need to improve on my first BB attempt to include JPG curves stored elsewhere; Picasa allows me only 800x500 px max resolution).
Should I ignore such a time period as not contributing to OSA, to desaturation, or to sleep fragmentation? Still I see a correlation between subjective accumulated sleep and the duration of sleep onset apnea cluster.
Last edited by AMUW on Wed Mar 23, 2011 2:28 pm, edited 10 times in total.
Moderate-severe OSA, ResMed S9 AutoSet EPR + H5i Humidifier, ResMed Masks: trying Swift FX Nasal Pillow, Mirage Nasal, Mirage Quatro or Quattro FX Full Face
ResMed SD card & USB adaptor, ResScan 3.10
ResMed SD card & USB adaptor, ResScan 3.10
Re: ResMed / ResScan interpretation challenge
Here's the flow from a typical sleep to wake transition. Both going to sleep and waking up is pretty much just like a light switch for me, either on or off. Seldom is there a 1/2 state, except when I'm trying to nap but am not really tired! Here you see a false apnea. My respiration always drops by about 1/3 to 1/2 when I go from sleep to wake. In going to sleep I'm usually zonked in 1 to 5 minutes after plopping down on the pillow. I looked over several days of graphs and find no cases of apneas within the hour or two after going to sleep, either CA or OA.AMUW wrote:does your final phase go in & out of consciousness, like my Sleep Onset?
Between clearly defined sleep and being awake and conscious I see a transition phase.

_________________
| Mask: AirFit™ P10 Nasal Pillow CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: Hose management - rubber band tied to casement window crank handle! Hey, it works! S/W is 3.13, not 3.7 |
- billbolton
- Posts: 2264
- Joined: Wed Jun 07, 2006 7:46 pm
- Location: Sydney, Australia
Re: ResMed / ResScan interpretation challenge
Basically, yes for OSA events and sleep fragmentation. Desaturations are desaturations, whenever they occur.AMUW wrote:Should I ignore such a time period as not contributing to OSA, to desaturation, or to sleep fragmentation?
If you have a RAMP time set on your machine you might want to try disabling it and going straight to the minimum set titration level, in case the lower treatment pressure during the ramp is creating some of the events you are observing.
Some more comments may be generally forthcoming from others, once you master posting a viewable chart
Cheers,
Bill
Re: ResMed / ResScan interpretation challenge
I struggled with similar symptoms for a long time, although my machine was not an auto-pressure one, so I just raised the pressure quite high. I managed the leaks by using (and modifying) a suitable mask. But I only resolved the problem recently by clearing up the upper airways (with a rather simple medical procedure). Have you exhausted all avenues in that direction?AMUW wrote: [...]
My therapy problem seems to be mainly cumulative nasal congestion after a couple of hours of sleep, which leads to upper airway restriction, then to flow limitation, which raises the Autoset pressure, creates leakage ... and so on in a vicious circle... on certain unpredictable nights.
[...]
McSleepy
_________________
| Machine: AirCurve™ 10 VAuto BiLevel Machine with HumidAir™ Heated Humidifier |
| Additional Comments: Previous machine: ResMed S9 VPAP Auto 25 BiLevel. Mask: Breeze with dilator pillows. Software: ResScan ver. 5.1 |
ResMed AirCurve 10 VAuto; Puritan-Bennett Breeze nasal pillow mask; healthy, active, middle-aged man; tall, athletic build; stomach sleeper; on CPAP since 2003; lives @ 5000 ft; surgically-corrected deviated septum and turbinates; regular nasal washes
Re: ResMed / ResScan interpretation challenge
I see what you mean idamtnboy; same for my awakening ... like maybe a horse switching rhythms from gallop to walk.idamtnboy wrote:Here's the flow from a typical sleep to wake transition. Both going to sleep and waking up is pretty much just like a light switch for me, either on or off.AMUW wrote:does your final phase go in & out of consciousness, like my Sleep Onset?
Between clearly defined sleep and being awake and conscious I see a transition phase.
My ResScan 3.10 doesn't have a separate Respiratory Rate display option, but I can count breaths per minute on the Flow curves.
BTW, have you noticed that your BPM curve doesn't change as sharply as one sees on the Flow curves: the smoothing probably has to do with the time window ResScan uses to calculate such a fundamental spectrum estimate.
My sleep onset certainly doesn't look quick at present when on CPAP. Here is another illustration, in addition to my previous post.
It can take me 10-30 min to go from 6-7 BPM to 13-14 BPM. I can go in and out of consciousness while I fall asleep, ResMed marks as apneas cessations in breath while still at the awake BPM. On other nights the curves can show a cluster of 20 apneas at sleep onset (not as periodic as in Cheyne-Stokes breathing).
Even later I can get hit with a few "events", and again it takes me a few minutes to regularize.
(Still working on a better resolution: the horizontal time scale is marked every 30 min, then for the fine scale at the bottom every 1 minute.)
Moderate-severe OSA, ResMed S9 AutoSet EPR + H5i Humidifier, ResMed Masks: trying Swift FX Nasal Pillow, Mirage Nasal, Mirage Quatro or Quattro FX Full Face
ResMed SD card & USB adaptor, ResScan 3.10
ResMed SD card & USB adaptor, ResScan 3.10