how to interpret Flow Limitation graphs
-
christinepi
- Posts: 75
- Joined: Sun Dec 12, 2010 2:18 pm
how to interpret Flow Limitation graphs
I finally found the Flow Limitation graph with the help of many friendly posters, and now I'd love some help with interpreting it.
On average, there are between 2 to 9 "bumps" in one hour. I don't know what the unit is called that describes their size or strength, but the bumps have a HEIGHT of ca 2 bars worth and stretch across horizontally, lasting ca 30 seconds. Does my description make any sense? I've learned that it's good when I see mounds and bad when it's flat. But I'm just not sure what exactly is meant by "mound": should it look like ONE mound spanning across the ENTIRE 8.5 hours of sleep, or many little mound shaped bumps, or what exactly? I know this is going to be hard to describe verbally, but please try to be as specific as possible...
Even though my AHI is always below 0.3, and has been since I started on CPAP 3 months ago, I still feel like a mess every day, just like always. From what I understand now, FL's are precursors to apneas/hypopneas. Maybe I have too many FL's to feel better and the Resmed just isn't recording those as apnic events. I guess my pressure is then still too low for them to be cleared together with the regular apneas. My recent titration study didn't look for RERA's, so I don't know what's up with those.
I tried to attach the graph w/o luck. Are there instructions somewhere on CPAPtalk on how to do that?
On average, there are between 2 to 9 "bumps" in one hour. I don't know what the unit is called that describes their size or strength, but the bumps have a HEIGHT of ca 2 bars worth and stretch across horizontally, lasting ca 30 seconds. Does my description make any sense? I've learned that it's good when I see mounds and bad when it's flat. But I'm just not sure what exactly is meant by "mound": should it look like ONE mound spanning across the ENTIRE 8.5 hours of sleep, or many little mound shaped bumps, or what exactly? I know this is going to be hard to describe verbally, but please try to be as specific as possible...
Even though my AHI is always below 0.3, and has been since I started on CPAP 3 months ago, I still feel like a mess every day, just like always. From what I understand now, FL's are precursors to apneas/hypopneas. Maybe I have too many FL's to feel better and the Resmed just isn't recording those as apnic events. I guess my pressure is then still too low for them to be cleared together with the regular apneas. My recent titration study didn't look for RERA's, so I don't know what's up with those.
I tried to attach the graph w/o luck. Are there instructions somewhere on CPAPtalk on how to do that?
_________________
| Mask: Mirage Quattro™ Full Face CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: Started 12/8/10; IP 14, EP 7 |
Re: how to interpret Flow Limitation graphs
Can't attach. Must use host site for the image.christinepi wrote: I tried to attach the graph w/o luck. Are there instructions somewhere on CPAPtalk on how to do that?
This is how I do it.
Open the image to full size so it is easily read.
I use Vista snipping tool to create a screen shot and crop the image at the same time.
Prt/scr key will also take a screen shot if using XP. If laptop is used sometimes the Fn key has to be pushed at the same time as the prt/scr key
I think windows 7 has the snipping tool.
Once the screen shot is created save it in jpg format.
Upload the image to a host site. I use Photobucket it is free, there are others.
Once the image is uploaded then copy the ENTIRE IMG address. Be sure to include the opening and closing IMG in brackets. Paste that copied address into a post here.
Use the preview button. If you can't see the image try again because if you can't see it we can't.
_________________
| Machine: AirCurve™ 10 VAuto BiLevel Machine with HumidAir™ Heated Humidifier |
| Additional Comments: Mask Bleep Eclipse https://bleepsleep.com/the-eclipse/ |
I may have to RISE but I refuse to SHINE.
Re: how to interpret Flow Limitation graphs
The smart ass answer is, "Good luck, 'cause you ain't gonna get any help!" The real answer, unfortunately, is much the same except in nicer words.christinepi wrote:I finally found the Flow Limitation graph with the help of many friendly posters, and now I'd love some help with interpreting it.
There are no good explanations what FL really means. It was discussed in this thread, viewtopic/t61287/viewtopic.php?f=1&t=60 ... on#p571528. Go to page 12 of the thread if the link doesn't take you directly there. In short the FL degree is an indicator, and apparently not a measure, of how much the upper airway passage is closed down and thus restricting, or limiting, the air flow. As to what the cause is, and what the impact is, apparently is quite elusive and no one really knows. That's why there are symbols and not numbers on the Y axis.
_________________
| Mask: AirFit™ P10 Nasal Pillow CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: Hose management - rubber band tied to casement window crank handle! Hey, it works! S/W is 3.13, not 3.7 |
-
christinepi
- Posts: 75
- Joined: Sun Dec 12, 2010 2:18 pm
Re: how to interpret Flow Limitation graphs
I'll check out the thread. And the fact that my "bumps" were in the lowest symbol area of the Y axis I guess means I'm in the more "mounded" area? Whatever that may ultimately mean...idamtnboy wrote:The smart ass answer is, "Good luck, 'cause you ain't gonna get any help!" The real answer, unfortunately, is much the same except in nicer words.christinepi wrote:I finally found the Flow Limitation graph with the help of many friendly posters, and now I'd love some help with interpreting it.
There are no good explanations what FL really means. It was discussed in this thread, viewtopic/t61287/viewtopic.php?f=1&t=60 ... on#p571528. Go to page 12 of the thread if the link doesn't take you directly there. In short the FL degree is an indicator, and apparently not a measure, of how much the upper airway passage is closed down and thus restricting, or limiting, the air flow. As to what the cause is, and what the impact is, apparently is quite elusive and no one really knows. That's why there are symbols and not numbers on the Y axis.
_________________
| Mask: Mirage Quattro™ Full Face CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: Started 12/8/10; IP 14, EP 7 |
Re: how to interpret Flow Limitation graphs
I think S9 Flow Limitation (FL) discussions almost inevitably become confusing as people interchangeably move back-and-forth among these three closely-interrelated topics---all about FL:
1) Flow Limitation- as it occurs in physiology
2) Flow Limitation- as it is reflected in the S9 “flow graphs" of individual breaths (pretty much the same as PSG flow graphs from which sleep labs log FL) and
3) Flow Limitation- as it is graphically interpreted/scored on the S9 “flow limitation graphs" (with graphing details that are proprietary and largely undisclosed)
This link, by Resmed, gives a good introduction of one and two above:
http://www.resmed.com/us/multimedia/und ... 40x380.swf
Note that two and three above are offered as separate graphs in the Resmed data set. That third one is obviously not a purely empirical graph and microanalysis is not suitable for that graph IMO. I think that third graph is best employed for purposes of trending and heuristically/visually comparing pre-interpreted FL severity from one night to the next.
Below are several flow-limitation types that we can directly observe on our S9 "flow graphs" that depict individual breaths (but not on the pre-interpreted S9 "flow limitation graphs"): http://chestjournal.chestpubs.org/content/119/1/37.full
1) Flow Limitation- as it occurs in physiology
2) Flow Limitation- as it is reflected in the S9 “flow graphs" of individual breaths (pretty much the same as PSG flow graphs from which sleep labs log FL) and
3) Flow Limitation- as it is graphically interpreted/scored on the S9 “flow limitation graphs" (with graphing details that are proprietary and largely undisclosed)
This link, by Resmed, gives a good introduction of one and two above:
http://www.resmed.com/us/multimedia/und ... 40x380.swf
Note that two and three above are offered as separate graphs in the Resmed data set. That third one is obviously not a purely empirical graph and microanalysis is not suitable for that graph IMO. I think that third graph is best employed for purposes of trending and heuristically/visually comparing pre-interpreted FL severity from one night to the next.
Below are several flow-limitation types that we can directly observe on our S9 "flow graphs" that depict individual breaths (but not on the pre-interpreted S9 "flow limitation graphs"): http://chestjournal.chestpubs.org/content/119/1/37.full
Re: how to interpret Flow Limitation graphs
In addition, what got really confusing (to me, anyway) occurred with the change in analysis from the S8 algorithm to S9. At first glance, everything appeared to be backwards. The solution was uncovered by LoQ in-SWS wrote:I think S9 Flow Limitation (FL) discussions almost inevitably become confusing as people interchangeably move back-and-forth among these three closely-interrelated topics---all about FL:
1) Flow Limitation- as it occurs in physiology
2) Flow Limitation- as it is reflected in the S9 “flow graphs" of individual breaths (pretty much the same as PSG flow graphs from which sleep labs log FL) and
3) Flow Limitation- as it is graphically interpreted/scored on the S9 “flow limitation graphs" (with graphing details that are proprietary and largely undisclosed)
You're Not in Kansas Anymore!
as we went from "Flattening" to "(Fuzzy) Flow Limitation":

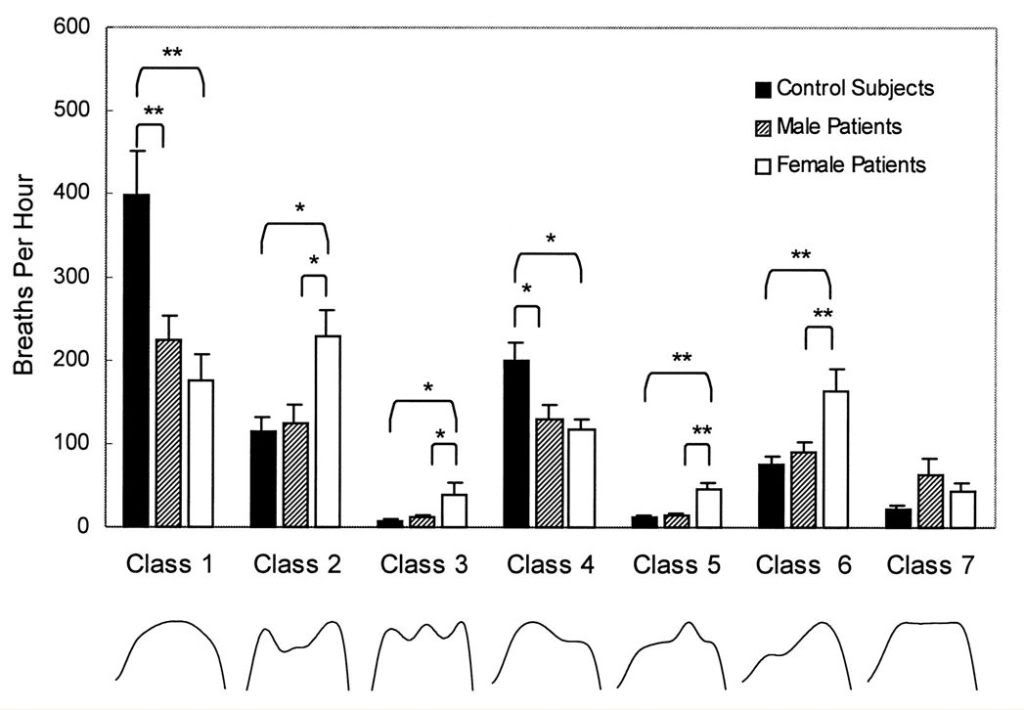
Additionally in addition (hopefully, without being redundant again), the Resmed algorithm seems to be very big on "M"s and "Chairs" (Classes 2 and 4 in -SWS's reference):
Last edited by NotMuffy on Sun Feb 02, 2014 4:20 am, edited 2 times in total.
"Don't Blame Me...You Took the Red Pill..."
Re: how to interpret Flow Limitation graphs
To -SWS and NotMuffy in particular:
To muddy the waters much further, any idea on how "bad" or how "long" the changes in the inspiratory part of the flow has to be before the PR System One decides to flag something as a "flow limitation" in Encore Viewer? I ask because the tick marks for "flow limitation" in Encore have never made any sense to me since I started out looking at continuous flow limitation graphs on the S9. And it was easy to correlate the "low" spots in ResScan 3.11 (where the FLAT Closed airway symbol was on the bottom of the graph) to, shall we say, stranger, less rounded inspiratory parts of the flow data itself. Since I never remember dropping below the "half-way" point between the "Open" rounded hump symbol and the "Closed" flat line symbol, I never worried too much about this. Although I did note that when I had flow limitations that corresponded to 75% of the way to "OPEN", that lasted any length of time (say 5--10 minutes or more), the S9 would increase pressure when in APAP mode.
And now on the PR S1 BiPAP, I've yet to see anything tagged as a "Flow Limitation" in Encore Viewer's detailed data. That's 2 1/2 months worth of FL index 0.0 and no tick marks on the Flow Limitation line. Haven't looked at anywhere near as much flow data since that requires an extra step now. But on bad nights, I do download the data into Encore Pro (on a different machine). And see some inspirations that look similar to ones that I used to see in ResScan's flow data during periods where the Flow Limitation curve was moving from the Open end towards the half-way to Closed part of the y-axis (and the S9 Auto algorithm frequently deciding to increase pressure). So I can't help but wonder: How ragged does the inspiration part of the flow data have to get (both in terms of shape and length of time) before the S1 scores it as a Flow Limitation?
To muddy the waters much further, any idea on how "bad" or how "long" the changes in the inspiratory part of the flow has to be before the PR System One decides to flag something as a "flow limitation" in Encore Viewer? I ask because the tick marks for "flow limitation" in Encore have never made any sense to me since I started out looking at continuous flow limitation graphs on the S9. And it was easy to correlate the "low" spots in ResScan 3.11 (where the FLAT Closed airway symbol was on the bottom of the graph) to, shall we say, stranger, less rounded inspiratory parts of the flow data itself. Since I never remember dropping below the "half-way" point between the "Open" rounded hump symbol and the "Closed" flat line symbol, I never worried too much about this. Although I did note that when I had flow limitations that corresponded to 75% of the way to "OPEN", that lasted any length of time (say 5--10 minutes or more), the S9 would increase pressure when in APAP mode.
And now on the PR S1 BiPAP, I've yet to see anything tagged as a "Flow Limitation" in Encore Viewer's detailed data. That's 2 1/2 months worth of FL index 0.0 and no tick marks on the Flow Limitation line. Haven't looked at anywhere near as much flow data since that requires an extra step now. But on bad nights, I do download the data into Encore Pro (on a different machine). And see some inspirations that look similar to ones that I used to see in ResScan's flow data during periods where the Flow Limitation curve was moving from the Open end towards the half-way to Closed part of the y-axis (and the S9 Auto algorithm frequently deciding to increase pressure). So I can't help but wonder: How ragged does the inspiration part of the flow data have to get (both in terms of shape and length of time) before the S1 scores it as a Flow Limitation?
_________________
| Machine: DreamStation BiPAP® Auto Machine |
| Mask: Swift™ FX Nasal Pillow CPAP Mask with Headgear |
| Additional Comments: PR System DreamStation and Humidifier. Max IPAP = 9, Min EPAP=4, Rise time setting = 3, minPS = 3, maxPS=5 |
Re: how to interpret Flow Limitation graphs
Why do you say that, if you don't mind my asking?NotMuffy wrote: . . . the Resmed algorithm seems to be very big on "M"s and "Chairs" (Classes 2 and 4 in -SWS's reference) . . .
I would have assumed the ResMed algorithm would be affected much more directly, in terms of response, by 3 (vibratory, snore-like, to my eye) and 7 (true flattening, as I understand it), if I was guessing.
Re: how to interpret Flow Limitation graphs
deleted
_________________
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: S9 Autoset machine; Ruby chinstrap under the mask straps; ResScan 5.6 |
Last edited by avi123 on Fri Mar 11, 2011 1:34 pm, edited 1 time in total.
see my recent set-up and Statistics:
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png
Re: how to interpret Flow Limitation graphs
Some auto-titrating-home-machine manufacturers (and one in particular) claim that their machines analyze the nature of the shape of the flow curve and react accordingly with pressure changes. In that sense, at least, it is not "academic" for the users of those home machines but is already being 'practiced.' Whether the machines react in a reasonable way based on that flow-curve analysis might be one basis for judging how "wishful" the thinking of the manufacturers. ResMed seems to consider that wish to be one that has already come true, as I understand it.avi123 wrote: . . . the whole issue in this case is sort of academic wishful thinking and not practicable. . . .
That said, I agree with you completely that shapes alone never tell the whole story--it is the effect of the breathing imperfections on the sleep of a particular patient that is the primary issue in every case, and that is mostly unknown outside an attended study at a lab/center.
As I understand it, the reason a ResMed auto watches the shape of the curve is not so much to estimate effect on sleep but to estimate likelihood of impending obstruction. It is my opinion that ResMed's manner of reporting on the breathing may be affected by that approach as well. So when patients then attempt to use the labels of the curves to estimate overall effectiveness of treatment, they may be using the data in a way that differs from how it may have been intended to be used--as a tool for trending.
Re: how to interpret Flow Limitation graphs
I'm a little bit inclined to agree. The other day I went to see my sleep doc. I actually talked to his right hand assistant, an FNP I think. Anyway, I asked her to take a look at a couple of nights of flow data. Well, they don't bother to download the hi-res data. Technician said it takes too long. As we were looking at the Resscan screen after she had tried to download the data, we moved by the Flow Limitation graph. The assistant made some comment about, "I don't know what that is." I would not characterize her as any kind of dummy. What this indicates to me is we on this forum may be hashing around issues that in the real world of sleep medicine actually are of relatively low priority. If my observation is valid, it would be interesting to know why such things as Flow Limitation are low priority.avi123 wrote:So the whole issue in this case is sort of academic wishful thinking and not practicable.
_________________
| Mask: AirFit™ P10 Nasal Pillow CPAP Mask with Headgear |
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: Hose management - rubber band tied to casement window crank handle! Hey, it works! S/W is 3.13, not 3.7 |
Re: how to interpret Flow Limitation graphs
I'm not sure that place exists yet.idamtnboy wrote: . . . the real world of sleep medicine . . .
To my way of thinking, there are at least three distinct worlds of OSA treatment, with little overlapping 'reality.'
1. Docs diagnose their patients and prescribe pressures in a manner that pleases insurance companies. The docs do so by using test results that others with technical knowledge generate for them. Most docs don't know diddly about home-treatment machines and have zero desire to know. That is how things mostly work in that world.
2. Manufacturers sell machines. To be allowed to do so in the U.S., the manufacturers have to (a) play the DME-insurance cartel game and (b) attempt to differentiate their products by innovating, or at least appearing to do so, and then patenting those 'innovations.' That is a second world. Docs don't know much about it. It ain't their bag.
3. Patients use the machines. That is the world I live in. We sometimes find ways to use the machines and the data in a manner that the docs and the manufacturers neither intended nor understand. We do so because it improves our sleep in tangible ways.
If manufacturers and docs want to know more about that developing third world, if you will, they can transport themselves from their worlds to ours, at least temporarily, by reading this board. I respect the docs and manufacturers who do so, whether they understand much of what they read here or not. (That last sentence is meant to show that the third world can be just as snarky and smug as the other two. )
Re: how to interpret Flow Limitation graphs
del
_________________
| Humidifier: S9™ Series H5i™ Heated Humidifier with Climate Control |
| Additional Comments: S9 Autoset machine; Ruby chinstrap under the mask straps; ResScan 5.6 |
Last edited by avi123 on Fri Mar 11, 2011 2:08 pm, edited 2 times in total.
see my recent set-up and Statistics:
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png
http://i.imgur.com/TewT8G9.png
see my recent ResScan treatment results:
http://i.imgur.com/3oia0EY.png
http://i.imgur.com/QEjvlVY.png
Re: how to interpret Flow Limitation graphs
avi,
Even the traditional "full PSG" doesn't do everything on your list:
Normal PSGs don't measure:
* Esophageal pressure (not unless there's a balloon down your throat---that's part of why many labs don't try to score RERAs)
* End-tidal CO2 (not the same as measuring blood O2 saturation; would require yet another sensor stuck up your nose.
* Arterial tonometry (while heart rhythms are recorded through the ECG, continuous measurement of blood pressure is not usually done)
And, if I recall correctly, during the titration study the flow from the CPAP is often used to record the air flow into and out of the nose. Certainly I don't remember any additional sensors being placed in my nostrils during my three titration studies and I wore pillows style masks for all three: So the pillows were sealed tight against the bottom of my nares.
Even the traditional "full PSG" doesn't do everything on your list:
Normal PSGs don't measure:
* Esophageal pressure (not unless there's a balloon down your throat---that's part of why many labs don't try to score RERAs)
* End-tidal CO2 (not the same as measuring blood O2 saturation; would require yet another sensor stuck up your nose.
* Arterial tonometry (while heart rhythms are recorded through the ECG, continuous measurement of blood pressure is not usually done)
And, if I recall correctly, during the titration study the flow from the CPAP is often used to record the air flow into and out of the nose. Certainly I don't remember any additional sensors being placed in my nostrils during my three titration studies and I wore pillows style masks for all three: So the pillows were sealed tight against the bottom of my nares.
_________________
| Machine: DreamStation BiPAP® Auto Machine |
| Mask: Swift™ FX Nasal Pillow CPAP Mask with Headgear |
| Additional Comments: PR System DreamStation and Humidifier. Max IPAP = 9, Min EPAP=4, Rise time setting = 3, minPS = 3, maxPS=5 |
Re: how to interpret Flow Limitation graphs
From LoQ's reference on FFL:jnk wrote:Why do you say that, if you don't mind my asking?NotMuffy wrote: . . . the Resmed algorithm seems to be very big on "M"s and "Chairs" (Classes 2 and 4 in -SWS's reference) . . .
The shape indices may be based on function(s) that ascertain the likelihood of the presence of M-shaped breathing patterns and/or chair-shaped breathing patterns.
"Don't Blame Me...You Took the Red Pill..."