Fitness Seeker wrote:Still trying to figure out what's wrong w/ me and the machine b4 I consider "other treatment options".
I have an XS Swift FX for her nasal pillows. My Qs:
1. Is the proper way to wear it is to have the silicone strap above the head like a headband and the velcro straps going horizontal completely horizontal? This is how i try to have it but it doesn't stablize. When i lie down the silicone strap keeps shifting and i constantly have to move it back onto my head. The velco strap seems too long. (I have an XS) and i can't tighten it; otherwise they straps will overlap and they won't stay in place anymore.
No, you've got the straps in the wrong place and it sounds like the top strap is too tight if it feels like a headband. Look at this image from cpap.talk's head with a Swift FX for Her:
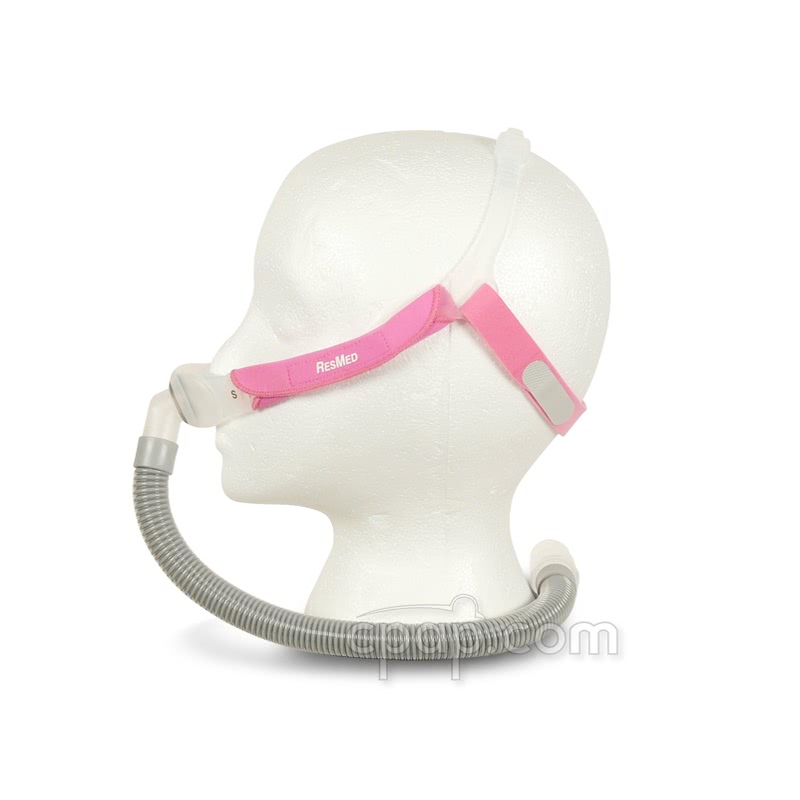
The top strap should be going more or less over the crown of your head. The back strap is lower down. It should not be horizontal. In practice, I find that the back strap often slides way up on my head (sometimes almost to the the slicone strap) without it necessarily breaking my pillows seal---at least when the pillows are new. As for the backstrap being too long, all I can think of a safety pin. But it could be that you are over tightening it in an effort to keep it horizontal.
2. When you put on this mask do u have to loosen the silicone strap? B/c i need to do this and then once it's on i tighten it. (otherwise i'd have leaks).
I think you are wearing the top strap too tight. I can easily get two fingers underneath that top strap (and that strap is also on top of a PadaCheek frame pad as well. I'd suggest NOT tightening it once it is on your head. This is a mask that should be worn really loose.
3. When you awake are you supposed to have marks on your face that stay for 1 hour?
NO! NO! NO! If the marks left by this mask are lasting an hour, you've got the mask WAY, WAY, WAY too tight. The mask should be sort of snug, but you should be able to get a finger under the straps on your cheeks without too much trouble.
Other Qs:
1. How do we know if the pressure is too much for us? (I'm trying to find the source of my intolerance). Can the DMEs adjust the pressure or do we need an MD's approval?
The DME will NOT adjust the pressure without a prescription change from the MD. As to how to tell if the pressure is too much? Well the
authorized way is to document (as in a log) just how much certain pressure-related things are bothering you and bring the list in and talk at length to the doc or PA that sees you. And ask whether they'd authorize a week or two of autotitration to see where your 90% or 95% pressure level settles in.
In my case, the PA authorized a switch to auto for a week of autotitration when I came into the office roughly 2 weeks into therapy on a semi-emergency meeting and looking like death warmed over. Hubby had called because he was alarmed at how quickly my daytime functioning was deteriorating and I'd already managed to write up a 10 page list of things I was concerned about not going well. The PA asked some kind of open ended question along the lines of: "Tell me what's going on and what's the hardest thing you're trying to cope with." I complained of the feeling of air getting into my eyes from my tear ducts, a rock hard stomach swollen to the size of a basketball each morning, and a truly terrifying dream of being a goose undergoing "forced-breathing"---i.e. being forced to take in more and more and more air until my lungs would pop and I'd wind up on the menu of a French restaurant in a morbid CPAPed-version of
foie gras It was the air-in-tear-ducts that really made the PA sit up and take notice.
Obviously another indication that the pressure may be too high is the emergence of significant numbers of central apneas----as in a CAI being consistently above 5.
For trying to sort out whether too much pressure is one of your issues, think carefully about this: Do you use the ramp? And how do you feel during the ramp period? Note that you don't want to be ramping up from 4cm to 10cm since the extra low pressure at the beginning may have some issues of its own. But if the ramp pressure is set to 2 or 3 cm less than your prescribed pressure, do you feel OK during the ramp period? And the DME
can change the beginning ramp pressure without needing the doc's ok, by the way. If you are using a Resmed S9, you won't be able to change the beginning ramp pressure without going into the clinical menu. But if you are using a PR System One, you should be able to change the beginning ramp pressure from the
patient's set up menu---unless the DME locked you out.
2. Does the apap have a bi-level capacity?
Some people claim the S9 AutoSet with EPR turned on acts like a bi-level. As someone who used that machine (unsucessfully) for 3 1/2 months before being switched over to a PR System One BiPAP, I'd say the S9 Autoset never felt like a bi-level
to me. Others mileage can and does vary. There have been several (long) threads where I've tried to explain why the S9 Autoset did not feel like a true bi-level to me and where others have adamantly maintained that the only difference between an S9 AutoSet with EPR and a true bi-level is that EPR is limited to a 3cm reduction in pressure at the beginning of the exhale. The thread with the most detailed information about the differences between how the pressure is reduced on exhale and increased on inhale on the various machine is at:
viewtopic.php?f=1&t=58773&st=0&sk=t&sd=a& . The interesting stuff starts on page 2 and the graphs in -SWS's posts are particularly useful in explaining the differences in how the S9 AutoSet with EPR, the S8 VPAP (bi-level), and the PR System One BiPAP each transition the pressure both from inhale to exhale and from exhale to inhale.
I was recommended by someone to get a bi-level but when I emailed the MD they said they don't "rescore" the sleep studies and that they the other machines are for "more severe apnea".
It's true that bi-levels are often used to treat other forms of apnea (not always sucessfully), but two rather common reasons for being put on a bi-level have nothing to do with the "severity" of the patient's apnea. First, many people are put on bi-level simply because their titrated pressure is very high (as in over 15 or 16) and the bi-level is often much more comfortable. Second, some folks do end up on bi-level because they are intolerant of straight cpap or apap even after some real effort has been made to make the therapy more tolerable. Take my own case for example: After 2 weeks of straight CPAP at 9cm, the PA authorized a week of autotitration which showed my 95% pressure level was around 7.8 or so and that I was much more comfortable with APAP than CPAP. But while switching to APAP running 4--8cm eliminated the air-in-eyes problem and somewhat helped the aerophagia, it did not bring the aerophagia down to truly tolerable levels. And I continued to crash and burn in terms of daytime symptoms. In other words, I was not responding to treatment (positively) even though my AHI was now well below 5. At the end of 7 or 8 miserable weeks, I was again in the PA's office (in another semi-emergency meeting) talking about the horrible aerophagia, the continuing crash and burn, and the insomnia monster that was growing large and fat. That was when she suggested a possible switch to bi-level and we scheduled the first bi-level titration. The long version of the story can be found here:
viewtopic.php?f=1&t=57491&p=541093&
Since your own doc seems to be reluctant to switch you to bi-level just because of possible pressure/tolerance issues, you might want to both read and provide your doc with a copy of
PR's Bi-Level Rescue Program
(particularly aerophagia and difficulty exhaling AGAINST the pressure with the machine's pressure relief set to its max
