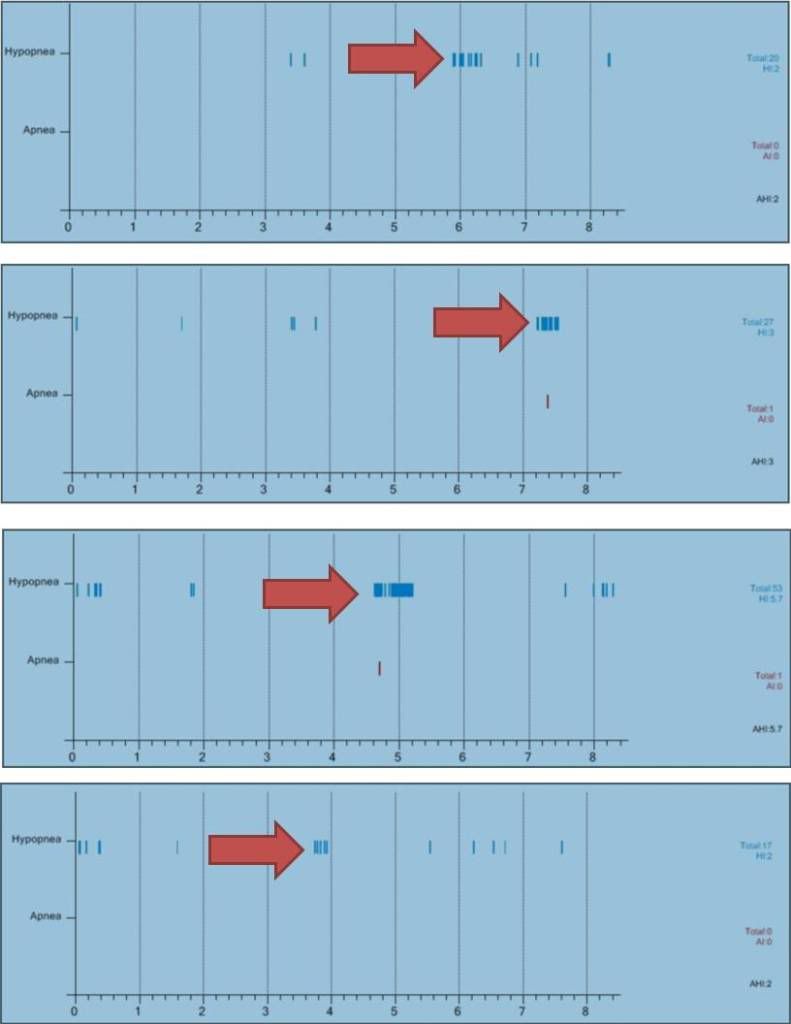
Zeke351 wrote: Do many of you get this/ What causes this?
There are a variety of possible explanations for that pattern. Looking at your report, we have no way of knowing if those are obstructive or central hypopneas. We don't know if they are based in sleep position or specific sleep stages. We don't know if they are based in a UARS type etiology (high upper airway resistance). We don't know if they are somewhat ordinary central-respiration instability---the kind that can occur during wake/sleep transitions throughout the night (I experience those). We don't know if you present slight central- or obesity-related hypoventilation at times---thus breathing patterns that your machine might score as hypopneas. We don't know if they are measurement artifacts or calculation type errors---since erratic breathing patterns can be algorithmically challenging to baseline regarding wildly changing recent-flow.
Some people here would experimentally raise their pressure to see if those hypopneas become better-addressed or even worsen. I advocate doing that with your doctor in the loop.
jonquiljo wrote: What do you call it when most of what you have are hypopneas? I am serious and cannot get a good answer from my sleep Dr. (or even Mr. Google).
Aside from what I mentioned above, they are sometimes just called "shallow breathing". The question is are they simply benign breathing patterns? Or are they instead associated with oxygen desaturations and/or sleep deterioration? Those kinds of breathing patterns, IMHO, are best diagnosed in a PSG. And, jonquiljo, I would also suggest trying to get your breathing pattern into Stanford since you live in the Bay area.
But even if you have mostly (confirmed) hypopneas versus apneas, it's still called:
http://www.google.com/search?hl=en&biw= ... =&gs_rfai=
Good luck to you both!